What is Diabetic Eye Disease?
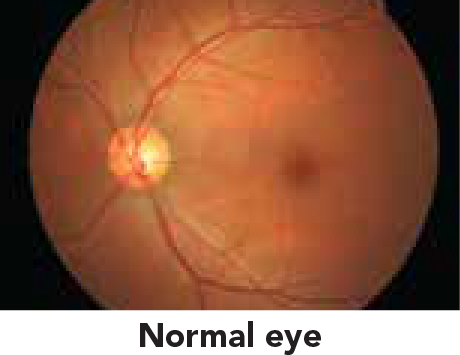
Diabetic eye disease is due to diabetes mellitus. The high sugar content in the bloodstream of diabetics indirectly affects the internal nerve layer of the eye
(retina) and can result in:
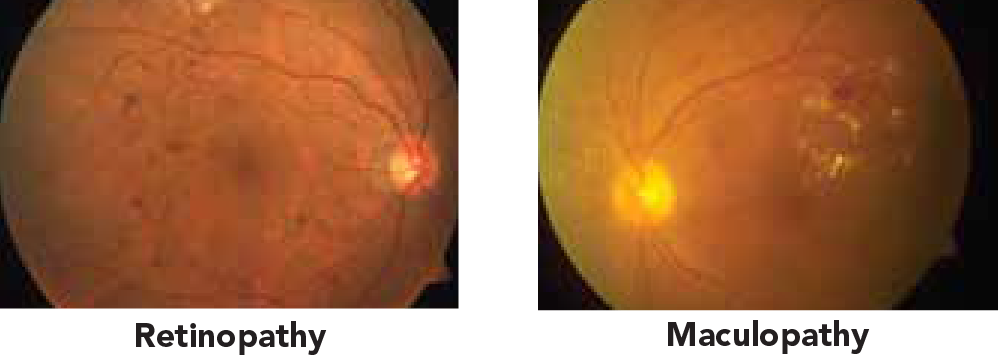
- Abnormal blood vessels
(retinopathy) with leakage and/or bleeding inside the eye, and/or
- Swelling of the central retina
(maculopathy).
Diabetic eye disease can eventually cause blindness if not treated.
Why Do I Need Laser Treatment?
You require laser treatment because your eyes have already been severely affected by diabetes. In some patients, vision may still be surprisingly good, even at this stage, but if treatment is delayed any further, there is a high likelihood of blindness in the future.
Research has proven convincingly that without treatment, the risk of losing vision may be up to twice as high. But laser treatment alone is not a “cure” for diabetic eye disease. Good blood sugar control with oral medication or insulin injections must continue.
Is There an Alternative to Laser Treatment?
Diabetic Maculopathy:
Anti-Vascular Endothelial Growth Factor (Anti-VEGF)
Injections into the eye (intravitreal injection) can help in reducing macular oedema. There are a number of drugs under this group which can be injected into the eye. However, these injections have to be administered on a monthly basis for good therapeutic response. These drugs may have local side effects such as infection, haemorrhage and/or systemic side effects such as stroke, heart attacks and gastric ulcers.
Steroids
Steroid injections into the eye also help in controlling macular oedema. They are available in the form of an injection or an implant which lasts for a few months.
Steroids do have a risk of developing an early cataract and glaucoma in addition to procedural risks of infection and haemorrhage. Your doctor would have discussed with you regarding the suitability of this treatment option.
Proliferative Diabetic Retinopathy
Anti-VEGF drugs have been used in some cases of proliferative diabetic retinopathy to control the retinopathy and prevent bleeding into the gel
(vitreous haemorrhage).
The effectiveness of anti-VEGF drugs in proliferative diabetic retinopathy given in multiple repeated injections has been shown to be comparable with panretinal photocoagulation in some of the recent clinical studies.
What is the Goal of Laser Treatment?
Laser treatment is done to reduce the chance of blindness and stabilize vision, NOT necessarily to improve vision.
- Those with maculopathy will require “focal” or “grid” laser treatment.
- Those with retinopathy will require “panretinal photocoagulation (PRP)”. Multiple sessions are usually needed.
Are There Side Effects From Laser Treatment?
These relatively minor side-effects are in exchange for the high likelihood of blindness if not treated.
-
Focal or
grid laser treatment may infrequently cause small areas of central visual blurring.
Risks:
Foveal Burn and Immediate Drop in Vision
During this treatment, patient needs to be very cooperative and must follow the surgeon’s instructions because a slight movement of the eye may result in inadvertent laser treatment to the fovea which is responsible for central vision.
Laser Scar Expansion and Late Decrease in Vision
Laser treated areas undergo scar formation and this may expand or extend beyond the intended areas treated. Some scars may extend to involve the fovea causing a decrease in vision.
Paracentral Scotoma
Laser procedures can cause a permanent damage to the retinal photoreceptors as well as neurons underlying the areas being treated. This in turn will produce a corresponding non-seeing area in the field of vision.
Choroidal Neovascularization
Repeated laser treatments to the same areas due to persistent maculopathy can injure the Bruchs’ membrane and choroidal vessels may grow and proliferate. This may also decrease vision.
Macular Pucker
Laser treatment near an epiretinal membrane may cause the membrane to contract and hence produce a macular pucker appearance which can also decrease the vision.
Lenticular and Corneal Burns
These refer to inadvertent laser damage to the lens or the cornea which may decrease vision.
-
PRP may cause dimmer vision especially at night, a smaller visual field, and in some cases, a temporary drop in vision.
Risks:
Dim Vision Especially in the Mesopic and Scotopic Condition
Laser treatment has a destructive effect on the retinal photoreceptors especially the rod photoreceptors which are concentrated more on the periphery where laser treatment is directed. This may cause difficulty in adapting to dim/dark conditions.
Narrowed Visual Field
Laser procedures can cause a permanent damage to the retinal photoreceptors as well as neurons underlying the areas being treated. This in turn will produce a corresponding non-seeing area in field of vision. In the case of panretinal photocoagulation, the area being affected is our peripheral field of vision which helps see things in the sides.
Transient Pain During and After Laser Treatment
Mild to moderate pain can usually be relieved with simple analgesics. However, patient experiencing severe/intolerable pain may request local anaesthesia (deep subtenon/ peribulbar lignocaine injection) on the premise that patient understood the risks of injection such as the possibility of collapse, globe perforation and haemorrhage.
-
Slight decrease in central vision and reduced colour perception
-
Vitreous haemorrhage
-
Retinal detachment
-
Vascular occlusion
-
Transient increase in IOP
-
Lenticular and corneal burns
What Can I Expect on the Day of Laser Treatment?
Laser treatment is not surgery, so no fasting is necessary. Laser treatment itself may take 5 to 20 minutes per eye, depending on the type of treatment required. However, be prepared to spend about 3 – 4 hours at the clinic, as preparation for laser treatment will take time.
-
Pupil dilation: Eye drops must be applied to open up your pupils to facilitate laser treatment. This may take at least 45 minutes or longer. Side effects of dilation include mildly blurred reading vision and glare in bright lights, and may last 3 – 6 hours.
-
If you are having panretinal photocoagulation (PRP): You may experience some pain during the treatment, but this is usually tolerable.
-
Things to remember on the day of treatment:
- Bring a light jacket as the clinic has to be kept cold for the laser machines to function well.
- Sunglasses will help reduce glare after treatment.
Do not drive as your vision may be blurred for several hours after treatment. Come with a companion so that he/she can take you home safely.
What Can I Expect After Laser Treatment?
You may be very dazzled by the laser light immediately after treatment and may have difficulty seeing for a short time. This usually improves after about 15 – 20 minutes but your vision may still remain blurred for 3 – 6 hours after that due to the pupil dilation, and of course the diabetic eye disease itself.
If you had PRP, you may experience a dull ache in the eye and a headache for the rest of the day. Light painkillers like panadol (if you have no allergies) are usually sufficient.
- You may go home immediately.
- No special after-care is required with diet and mobility.
Please do not drive after treatment.
- necessary - work can resume the next day.
- A follow-up appointment will be given to monitor the disease and plan the next step.
- The majority of patients will not experience any improvement in vision after laser treatment.
Remember: the main goal of laser treatment in diabetes is to reduce the risk of further deterioration and subsequent blindness. In a few patients, internal bleeding and swelling can be dramatically reversed by the laser treatment, and only in these cases, mild improvement of vision may occur.