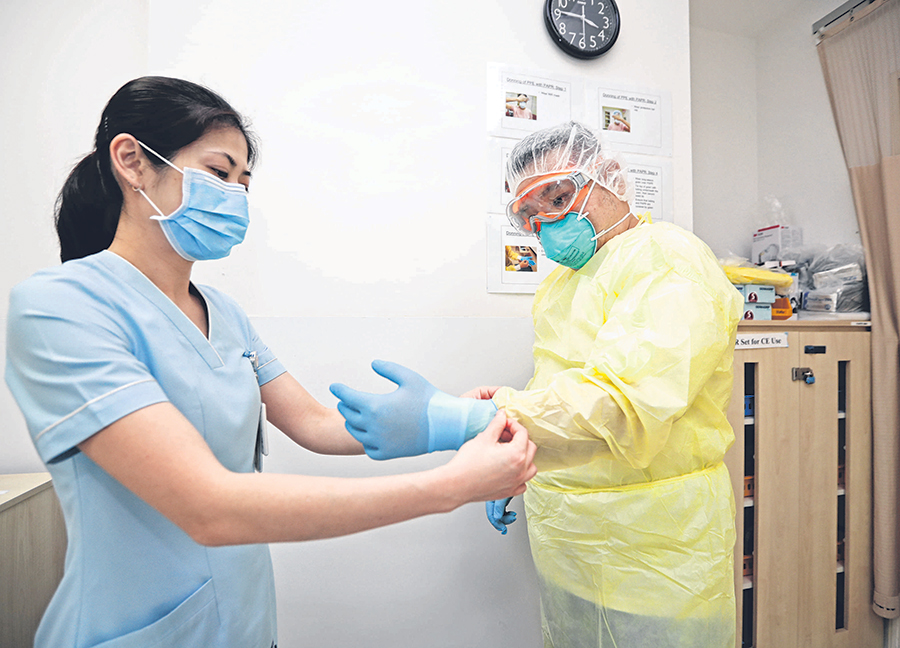
 Mr Christopher Soh, assistant director of nursing at Tan Tock Seng Hospital’s emergency department, putting on protective personal equipment while his wife, Ms Tina See, an infection prevention and control nurse, ensures the proper steps are followed. ST PHOTOS: GIN TAY
Mr Christopher Soh, assistant director of nursing at Tan Tock Seng Hospital’s emergency department, putting on protective personal equipment while his wife, Ms Tina See, an infection prevention and control nurse, ensures the proper steps are followed. ST PHOTOS: GIN TAY
The Sunday Times (15 March 2020)
The Sunday Times finds out how they support each other and keep their families safe, and what their greatest worries are
The scale of the fight against the coronavirus outbreak, which the World Health Organisation recently declared a pandemic, surprised most medical professionals.
For Dr Koh Li Wearn, a senior consultant at Tan Tock Seng Hospital (TTSH), a big meeting in late January involving senior hospital management was revelatory.
“I thought, oh my goodness, so this is what people had been preparing for all this time,” she says.
She realised at the meeting that “the whole hospital infrastructure” was involved – “the facilities team, supply chains, the laundry department, the people who man the entrances and exits, and those involved in visitor experience”.
Medical staff at TTSH have been preparing for the possibility of such an outbreak for years.
Mr Christopher Soh, assistant director of nursing in TTSH’s emergency department, says the hospital has been undertaking “active preparations” since the ebola outbreak (2014 to 2016) in West Africa.
The emphasis is on teamwork, say Dr Koh and Mr Soh, whose spouses are battling alongside them, albeit in different roles, in the war against the coronavirus.
At the end of the day, Dr Koh stresses that the fight extends beyond doctors and nurses, either singly or as couples such as herself and her husband.
It includes “the auntie who stands at the bottom of the escalator, cleaning it with disinfectant, just to keep the place going. She’s the hero”, she says.
Nurses soldier on
When the coronavirus outbreak erupted, Mr Christopher Soh’s first thought was: “Here we go again.”
Mr Soh, assistant director of nursing in the emergency department of Tan Tock Seng Hospital (TTSH), and his wife, a fellow nurse, soldiered through the severe acute respiratory syndrome (Sars) outbreak in 2003 and H1N1 in 2009.
This time, he says, the patient profile is different compared with that of previous outbreaks. For instance, a stroke victim and a man with a fractured foot were admitted to the National Centre for Infectious Diseases (NCID). Both had to be treated for their trauma conditions in addition to respiratory symptoms.
In this way, the screening centre has become “like a second emergency department”, he says. His affinity for emergency medicine has been honed in disaster.
He volunteered as a medic in Trincomalee, Sri Lanka, after the 2004 Indian Ocean tsunami struck. Fishing trawlers beached 10km inland after the tsunami made a deep impression on him.
His experience has given him insights into “what is important in a crisis, such as assuring your staff they are in safe hands and being transparent in communication”. His wife, Ms Tina See, is a nurse clinician in the department of infection prevention and control.
The couple, both 43, have a 13-yearold son and a 10-year-old daughter.
He empathises with the fear of contagion some of his staff feel.
“My fear is not specifically to do with Covid-19, but in dealing with any infectious pathogen. This is my calling and I see it as part of the job, but the fear is of taking back infection to my loved ones,” he says. His wife does not share this anxiety as her job is “making sure the healthcare workers are safe”.
The TTSH Infection Prevention and Control team, of which she is a part, conducts N95 mask-fitting training for healthcare workers and ensures compliance with infection control and related practices.
Examples of these practices include good hand hygiene and the proper donning of personal protective equipment.
Mindful of the unease some may feel in the presence of front-line health workers, the couple stay away from social functions. Mr Soh says: “We try not to take part in dinners or social events. Others may feel uncomfortable around us, but they may not say it.”
Because the couple have been in nursing for more than 20 years, they have an “unspoken” understanding of what to do if one of them falls ill.
They have designated the master bedroom as a segregation zone if needed. And their children have learnt not to be anxious.
Ms See says: “I asked my children if they were worried and they said ‘no’. I asked if they felt proud. The girl said she didn’t know, while the boy said he was ‘a bit proud’ of us.”
 Dr Koh Li Wearn and her husband, Dr Ho Eu Chin, looking at artwork and notes of encouragement from members of the public, schools and volunteer organisations. The couple made sacrifices at home when they responded to a call for healthcare workers to serve at the National Centre for Infectious Diseases.
Dr Koh Li Wearn and her husband, Dr Ho Eu Chin, looking at artwork and notes of encouragement from members of the public, schools and volunteer organisations. The couple made sacrifices at home when they responded to a call for healthcare workers to serve at the National Centre for Infectious Diseases.
Doctors on the front line
After Dr Koh Li Wearn, 44, signed up to volunteer for front-line duty against the coronavirus in January, she went home to find out her husband had done the same thing.
Echoing her husband’s views, Dr Koh, a senior consultant in the rheumatology, allergy and immunology department, said: “I wanted to know what the enemy was like.
When you don’t know, your imagination makes it worse.
“The junior doctors under me were on a roster to go in. They didn’t have a choice. I couldn’t send them in if I didn’t go in myself.”
Both she and her husband, Dr Ho Eu Chin, a senior ENT (ear, nose and throat) consultant, work at Tan Tock Seng Hospital (TTSH).
She was rostered at the isolation ward at the National Centre for Infectious Diseases (NCID) for two weeks, from Jan 31 to Feb 13.
Dr Ho was at the NCID Screening Centre from Feb 10 to 19 and will be rostered again later this month.
The NCID, a 330-bed facility designed to strengthen Singapore’s capabilities in infectious disease management and prevention, is located next to TTSH.
As part of her roster duty included examining coronavirus patients daily, Dr Koh learnt to cope with the fear of infection.
She heeded the advice of experienced peers.
“My colleague said, ‘Trust the protective equipment.’ He offered me tips. Every time I tried to take off the mask, my glasses would fall off. He taught me to put the mask strap and goggles on in a certain way to avoid that.”
Medical professionals have to put on protective personal equipment (PPE) when dealing with suspected and confirmed coronavirus cases.
The protective gear includes an N95 mask, goggles, a long-sleeved gown, a shower cap and gloves made of synthetic rubber.
The PPE affords safety, but also creates distance, as facial expressions and non-verbal cues are hidden.
Dr Ho says: “The patients also wear masks. I had to try harder to communicate well with them, to slow down and repeat myself, and to convey reassurance and empathy.”
This was especially important when the patients spoke another language, such as some foreign workers whose English was rudimentary.
“You sense they are fearful of losing their job. They’ll say, ‘Oh, my boss won’t like this’,” he adds.
Even though the couple has made sacrifices at home, their thoughts are always with the patients.
For a month, during the two weeks she was on duty and for two weeks after that, Dr Koh slept in a spare room, apart from Dr Ho. They did not hug and kiss their children.
Their 13-year-old son understood why, but their nine-year-old daughter did not quite understand the change in her usually affectionate parents.
Dr Ho says: “I sometimes worked night shifts, which meant I could fetch her from school. She wanted to hug me, but I said, ‘No hugs.’ Being able to pick her up made my day, though.”
Dr Koh says social distancing at home was tough. “Although I couldn’t hug and kiss them, I sat with them at mealtimes – they were at one end of the table, I was at the other. It made me realise how much harder it is for people in isolation, away from their loved ones.”
She adds: “I’m glad I did go into the isolation ward. I feel less daunted by the coronavirus.”