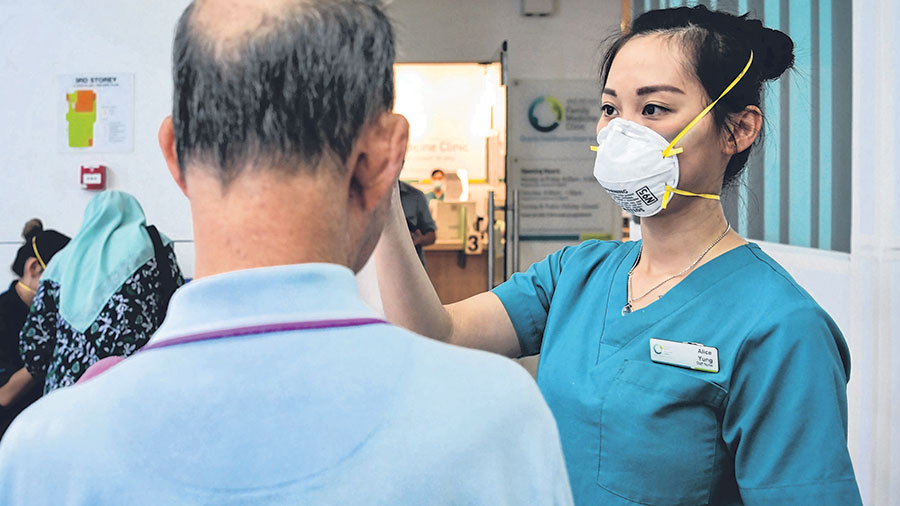
 As the population ages rapidly, nurses will have to step up to a much bigger role as architects of care, influencing patients, families and other stakeholders in the area of care options, making decisions on the best care for patients and coordinating care delivery with various providers.
As the population ages rapidly, nurses will have to step up to a much bigger role as architects of care, influencing patients, families and other stakeholders in the area of care options, making decisions on the best care for patients and coordinating care delivery with various providers.
ST PHOTO: KUA CHEE SIONG
The Straits Times (26 September 2020)
A veteran nurse has seen how nursing has evolved over the decades, from basic nursing duties to redesigning hospital wards so nurses spend less time walking and more time by patients’ bedsides. The next phase: nurses managing care for ageing patients in the community.
The ongoing Covid-19 pandemic has a silver lining: It has raised awareness and appreciation of the role of healthcare workers, including nurses. This is one reason why more people are switching to nursing mid-career.
As a veteran nurse, I see this as a welcome move because nursing can benefit from the influx of professionals with diverse experience.
At the same time, these mid-career adults will find that nursing these days offers a wide range of roles, far beyond that of the clinical care in hospital wards that most people are familiar with today.
In my 24 years as a nurse, I have seen the growth of nursing as a profession and, in my modest way, contributed to this growth. I was involved in three changes to improve the nursing profession over two decades.
The first change was more empowerment through reduced hierarchical structure; second, more pathways for nursing beyond task-based roles; and third, involving nurses in training others (support staff, caregivers and patients) to take on tasks that were once performed only by nurses.
From student nurse to nurse administrator
My story began when I was a student in the United Kingdom from 1991 to 1995, at the University of Manchester. I spent my final year of studies as a community nurse, forging friendships with patients and linking them up with the follow-up care required.
I enjoyed the close interactions and the feeling of efficacy that came from being able to help them with my nursing skills. This was the precise reason why I had wanted to be a nurse in the first place.
In 1996, I returned to Singapore and took up a position as a registered nurse at Tan Tock Seng Hospital, hoping to repeat the experience of professional autonomy I had enjoyed abroad.
But my first three years in the general wards and intensive care unit (ICU) were spent on honing my clinical (practical) skills instead, and I had to oversee the care of more than 12 patients in each shift.
The task-oriented aspects of the job helped me understand why the public in Singapore viewed nursing as an “unglamorous” job involving hygiene care, and why patients and their families preferred to discuss important decisions with doctors.
As a junior nurse, I observed that nurses received more compliments from patients and families about their care experience than doctors and allied health professionals did.
This is unique to a nurse’s calling and profession.
After three years in the wards, I took up an opportunity to go on the nursing administration track in 1999, hoping to effect greater change.
Over the decades, I found that two concepts are useful in understanding the changing role of nurses: the idea of nurses beyond nursing; and nursing beyond nurses.
“Nurses beyond nursing” means upskilling nurses to achieve deeper professional competencies as advanced practice nurses, nurse clinicians, ward resource nurses, principal nurses and community nurses.
This involves redefining and strengthening the nurse’s role as a first responder and knowledgeable patient and family advocate. In the near future, we can expect to see nurses undertaking more clinical decisions and initiating more orders of investigation and intervention that are usually taken on by doctors.
This is the future of nursing: learning across disciplines and gaining trans-disciplinary skills – which means the nurse may be equipped with the competencies of the doctor, pharmacist and therapist to better manage and integrate care for the patient, especially in an ageing population where we see more seniors with complex conditions.
“Nursing beyond nurses” empowers support staff like healthcare assistants, health attendants and patient service associates to take on value-added roles like venepuncture (puncturing a vein to draw blood), running electrocardiogram and urine flow management tests or the removal of intravenous cannulae (flexible tubes inserted into veins).
Renovating for the future
Another interesting project I was involved in was the Ward of the Future (WOF) innovation project in 2010.
What started out as a renovation project to upgrade wards became the transformation of inpatient nursing. This was against a backdrop where nursing work was notoriously exhausting, both physically and emotionally.
In our initial studies, we shadowed a group of nurses for an entire shift over two weeks. We found that nurses spent most of their time away from the bedside – each nurse could walk up to 8km in each shift and yet spend only about 10 per cent of his shift hours in direct care with the patient and/or the patient’s family.
Such a disengaging experience aggravated the nurses’ sense of physical fatigue and became one of the top reasons for dissatisfaction at work. Consequently, it contributed to a fairly high level of attrition among nurses.
One key change was to redesign the layout of the ward to improve the nurses’ line of sight of patients, to enable more direct patient care.
In our bid to improve line of sight for the nurses, we learnt that patients also expressed their comfort about being able to see a nurse nearby, thus making the environment conducive for healing.
The WOF project was awarded the Public Service’s Best Practice Award for Organisational Development in 2014.
Over three years, significant changes included improvements in response time to patients’ needs (by about 25 per cent) and direct care time for nurses (from 10 per cent to 30 per cent).
Another project to get nurses across the ranks involved in coming up with good ideas to improve their practice saw good results. One innovation was having new hospital beds fitted with a motorised fifth wheel and a built-in weighing scale, saving half the transfer time and energy to carry a patient off the bed to be weighed.
Another innovation was a one-piece hospital gown with buttons on the sides near the shoulders, and two straps at the back, for ICU patients. This special design allows lines and tubes to be accessed easily and for pyjamas to be changed in less time.
Nurses in the wards also had an idea of specially designing hand mittens that are cushioned and fastened with zips, for patients with dementia or delirium. This prevents them from pulling out their tubes or catheters if they become agitated or restless.
The future of nursing
In recent years, we have progressively removed unnecessary manual tasks from nurses’ care responsibilities. But core nursing roles such as basic hygiene care that cannot be replaced or automated in the near future will remain important tasks.
As nurses, we see this as part of being a “complete” healer – to influence and decide the path of healing for the patient, and then be a partner of the patient and family all the way in their healing journey, even when cure is not (immediately) imminent.
But as the population ages rapidly, nurses will have to step up to a much bigger role as architects of care, influencing patients, families and other stakeholders in the area of care options, making decisions on the best care for patients and coordinating care delivery with various providers.
In Singapore, doctors, not nurses, usually perform this role of deciding on and structuring care for patients.
But this has to change in order to achieve a sustainable care model in a rapidly ageing population. This is because care interventions are not as straightforward as before, and may require more mutual goal settings and multiple adjustments along the healing process.
After all, many people, including myself, would prefer to age in place and within our home and neighbourhood. For example, if my health condition is not too complex, I would prefer to see only one healthcare practitioner who is familiar with my health profile so that costs remain affordable.
As I see it, the nurse fits this role best. This is because nurses are at almost every touch point of the patient’s healthcare journey, and we are increasingly competent.
Nurses in Singapore are more than ready to play a pivotal role in overcoming challenges and transforming the way healthcare is to be delivered in the future.
If we can keep our focus on making a difference in the patient’s healing process, I firmly believe we can achieve more and step up, as shown by how we have demonstrated courage, wisdom and steadfastness in facing all disease outbreaks so far.