The inside of the eye is lined at the back by a layer of delicate nerve tissue called the retina. The retina is like the film of a camera that converts the light into images, and sends them to the brain. The macula is a small area at the centre of the retina which is used to see fine details for activities such as reading and sewing.
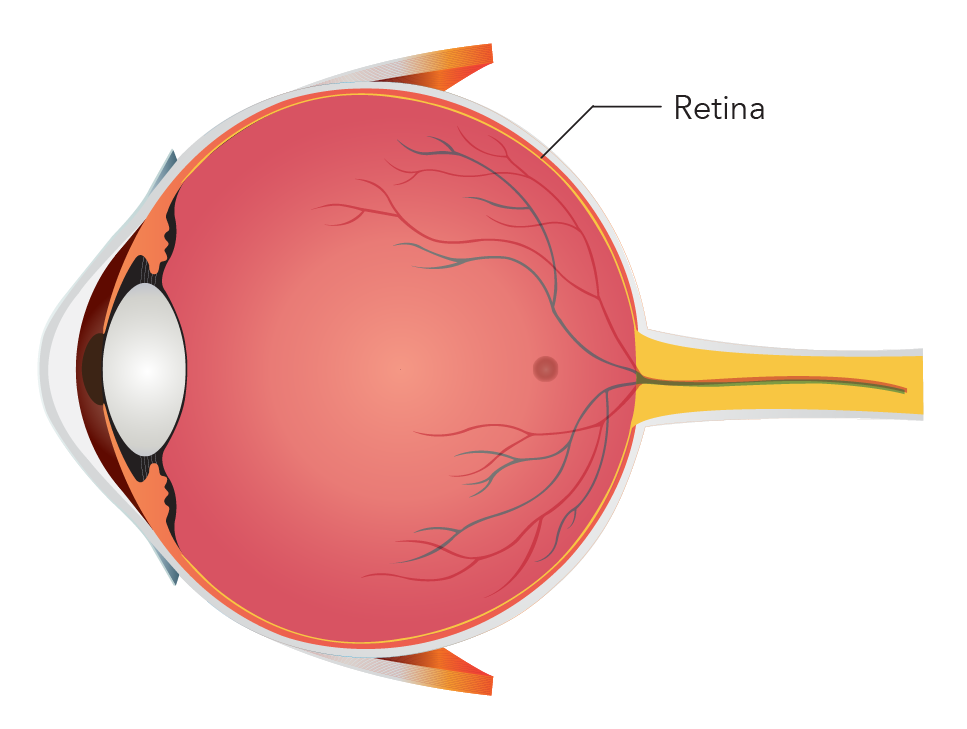
Illustration of a normal eyeball.
What is Age-Related Macular Degeneration (AMD)?
Deterioration or breakdown of the macula (central partof the retina) can occur with age. This causes the delicate cells to become damaged and stop working. Central vision is affected such that a dark patch blocksthe centre of the visual field. However, AMD almost never leads to total blindness. Patients with macular degeneration will usually have enough peripheral vision (vision outside the central area of gaze) to get around to remain independent.

AMD is the leading cause of legal blindness in the over 65 year age group in developed countries of the west. Some patients develop AMD even before they reach the age of 60.
As the population in Singapore is ageing, AMD is becoming a significant cause of blindness here as well.
Broadly, there are two types of AMD:
Dry AMD
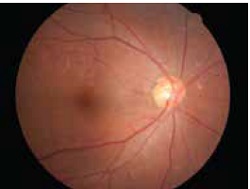
This form of AMD makes up about 90% of AMD. In this type, there is deposition of waste products in the macular region, followed by degeneration of the retinal cells. Although there is no known effective treatment for dry AMD, vision is usually preserved until very advanced stages.
Wet (Exudative) AMD:
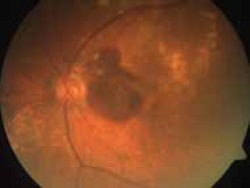
The development of abnormal blood vessels (known aschoroidal neovascularization) under the retina can lead to fluid and protein leakage or bleeding. The loss of vision is usually more severe than dry AMD, especially if scarring has occurred. Early treatment helps to prevent rapid progression of the disease. Another form of wet AMD which particularly affects Asians is idiopathicpolypoidal choroidal vasculopathy (PCV).
What are the Symptoms?
In the early stages, the central vision of the eye may beblurred or distorted, with objects looking an unusual sizeor shape and straight lines appearing wavy or fuzzy. This may happen quickly or develop over several months.This can be detected by using an Amsler gridmonitoring chart.
Instructions: This chart should be held 30 cm from theeye. You may wear your reading glasses if necessary. Test one eye a time by blocking the other eye with yourpalm without pressing on it. Look directly at the centraldot with the uncovered eye.
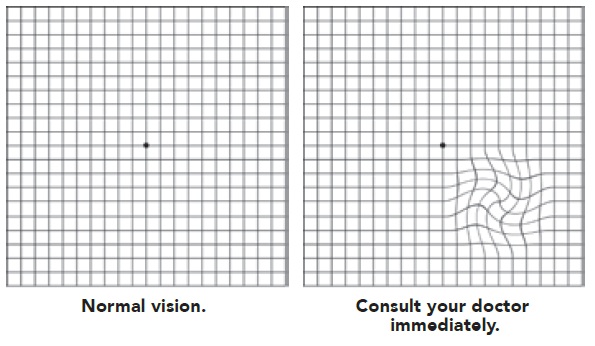
Because macular degeneration affects the centre of the retina, people with advanced AMD will often notice a blank patch or dark spot in the centre of their sight. This makes reading, writing and recognising small objects orfaces very difficult.
What are the Risk Factors for AMD?
- Age more than 60 years old
- Smoking
- Family history of AMD
- Obesity
- Gender (Women)
- Cardiovascular disease
- Poor dietary intake
What Treatments are Available?
Early detection is necessary for early diagnosis and treatment, to increase the chances of improving vision.
The types of treatment available for AMD
- Laser photocoagulation (A procedure done wherethermal laser is applied.)
- Photodynamic therapy with Verteporfin (A non-thermallaser procedure applied to activate an intravenous drugto close the abnormal blood vessels)
- Intravitreal drugs (injected directly into the eye) e.g.anti-vascular endothelial growth factor (VEGF)(Lucentis®, Eylea®, Avastin®)
- Surgical intervention to displace blood (released byabnormal new vessels) under the macula using aninjection of tissue
High risk patients are offered antioxidant supplementscontaining vitamins C, E, Zinc, Copper, Zeaxanthin and Lutein to prevent progression of dry to wet AMD.It is also advisable to stop smoking, because smoking hasbeen identified as a risk factor for AMD. In the advanced form of the disease, low vision aids suchas mini telescopes and magnifying glasses may help somepatients.
What Should I Do if I Think I Have AMD?
Anyone who develops blurring of central vision shouldvisit a retinal specialist (an eye doctor specialised in retinal diseases) as soon as possible. Tests may be required to help in diagnosis and assessment of the condition. Treatment will be based on the findings of the examination and investigations. Your retinal specialist will be the best person to explain the problem and the treatment options.