What is the Episcleritis and Scleritis?
The sclera is the white outermost coat of the eyeball. It forms the four-fifths of the tough outer wall of the eyeball (red arrow) and the other one-fifth is comprised of the crystal clear, watch-glass like structure in the front of the eye through which we see, the cornea (black arrow).
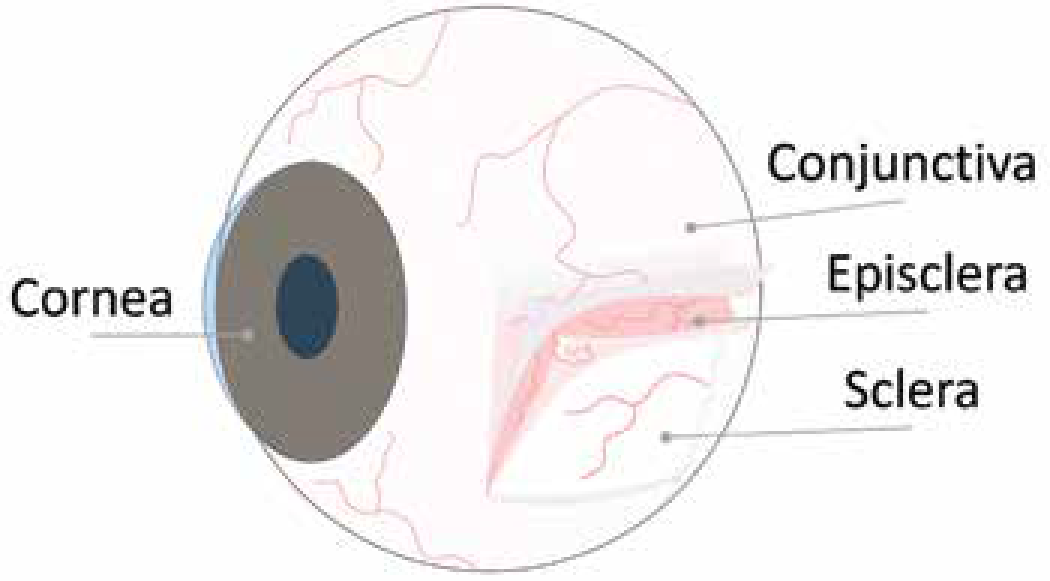
Illustration showing the parts of the eye containing the cornea, conjunctiva, episclera and sclera.
On the front side of the eyeball,the sclera is covered by a thin transparent membrane, which is known as conjunctiva.
In between conjunctiva and sclera, there is another important layer, which is known as episclera. Episclera is actually a part of the sclera.
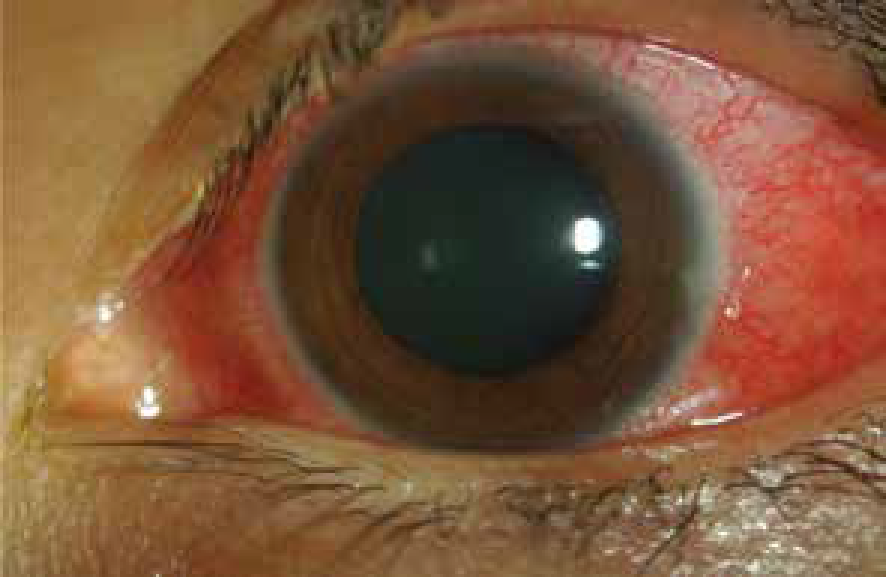
A red eye due to scleritis.
What is Episcleritis and Scleritis?
Inflammation of the sclera can be divided into two broad categories namely episcleritis and scleritis.
Episcleritis and scleritis are two important differential diagnoses for a patient with red eye.
While episcleritis is a self-limiting condition, scleritis is often associated with systemic autoimmune disease and may lead to severe complications and blindness.
A systematic approach is imperative in monitoring and management of patients with episcleritis and scleritis.
Both the conditions need to be differentiated from other causes of red eye such as conjunctivitis, acute anterior uveitis, acute congestive angle closure glaucoma or any intraocular infections.
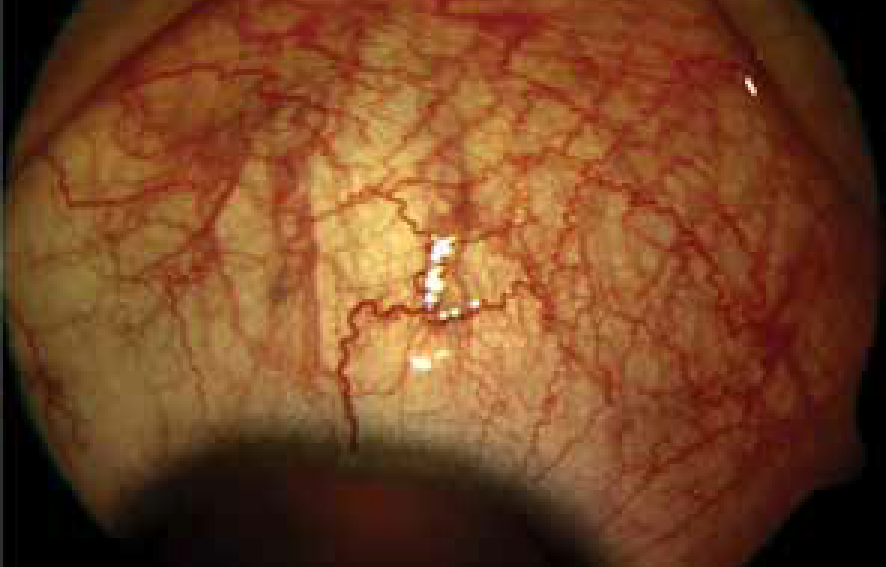
An eye with episcleritis.
What are the symptoms of Episcleritis and Scleritis?
Episcleritis and scleritis present with red eye, prickly eyes of variable duration.
Episcleritis is associated with discomfort to mild pain, foreign body sensation, while scleritis is usually associated with mild to severe pain.
Pain in scleritis can be quite severe to wake the patient up from deep sleep. Most commonly, both the conditions do not present with decreased visual acuity but scleritis can lead to blurred vision to marked visual loss.
What are the other systems involved with Episcleritis and Scleritis?
Episcleritis is a benign condition not associated with any specific systemic involvement but scleritis can be associated with systemic autoimmune diseases like Rheumatoid arthritis and other forms of collagen vascular disorders.
What are the investigations required for Episcleritis and Scleritis?
Episcleritis typically does not require any investigations while a patient with scleritis will require extensive laboratory investigations to rule out any underlying associated systemic disease.
What is the treatment of Episcleritis and Scleritis?
Episcleritis is a self-resolving disease and can be managed by topical eye drops. In contrast, treatment of scleritis depends on the stage of disease. In early stage, oral non-steroidal anti-inflammatory drugs (like Indomethacin) can be beneficial. While in severe or advanced stages, oral steroids or steroid-sparing immunosuppressive agents may be required. Some cases of severe scleritis may require stronger biologic agents.
What are the complications of Episcleritis and Scleritis?
Episcleritis usually resolves without any complications but can be recurrent.
Scleritis can potentially lead to vision loss, and can be recurrent in nature. It can also be associated with
- Increased intraocular pressure, anterior chamber inflammation and in some cases with corneal involvement.
- In some cases, it can lead to melting of the sclera with dehiscence of the uveal structures.
- Importantly it can be associated with severe lifethreatening conditions.
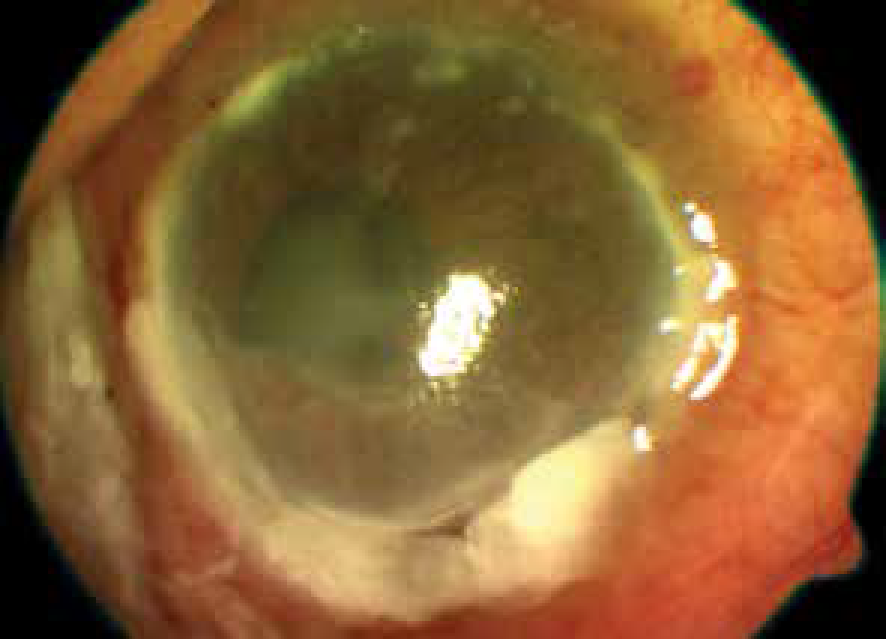
A case of scleritis with peripheral corneal melting (complication of scleritis).