Download English PDF, 675KB, PDF
Hydration & Nutrition at the End of Life
Many of us may have concerns about our loved one not being able to take any thing orally when they become too drowsy or develop swallowing difficulties. Witnessing a loved one eating minimally can be distressing and we hope that the follow information will help allay your concerns.
Clinically-Assisted Nutrition & Hydration
Some alternative ways to provide nutrition and hydration artificially includes
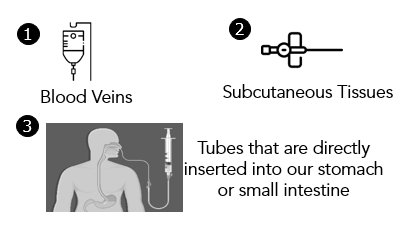
When is CANH recommended for patients?
- When he/she has a treatable illness like food poisoning
- When one is required to fast for a planned operation
Is Clinically-Assisted Nutrition and Hydration Recommended at the End of Life?
Generally, we do not recommend these alternatives for terminally ill patients because of:
-
Lack of hunger
Your loved one is usually unable to feel hunger at the end of life due to a change in his/her body’s physiological needs -
Inability to absorb fluids at the terminal phase
AHN often causes generalised swelling, fluid build-up in the lungs, increase in phlegm and vomiting. These fluids often worsen breathlessness. -
Physical restraints may be required to keep the feeding tube in place
Feeding tubes that are inserted to deliver AHN often cause discomfort, and your loved one may attempt to remove them. This affects his/her dignity and increases frustration experienced by your loved one.
What Can I Do to Help My Loved One?
You are encouraged to use oral swabs for the following purposes:
- Clean and moisten your loved one’s mouth
- Feed your loved one his/her favourite drink.
Oral swabs are soft sponges that ensure gentle cleaning of the mouth
Instructions on Using Oral Swabs:

1. Pour his/her preferred beverage into a cup. Soak the oral swab briefly.
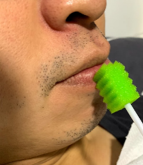
2. Dab his/her lips.
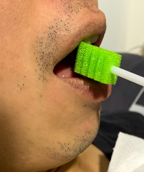
3. Proceed to clean his/her mouth and allow him/her to suck the sponge. Stop immediately if your loved one chokes or coughs.
Will My Loved One Die Faster Without Food and Drink?
No, he/she will not. Studies conducted on patients at the advanced stage of their cancer have proven that drips and milk feeds through tubes do not prolong survival nor improve quality of life.
When doctors do not recommend alternative feeding methods, it is always in the best interest of your loved one’s comfort and wellbeing. The palliative care team will constantly assess patients to ensure that sufficient medications are given to relieve any symptoms causing discomfort or distress.
It also does not mean that the medical team has abandoned or given up on your loved one. The team will pay careful attention to meticulous and regular oral care (lubricating the lips and keeping his/her mouth moist) instead, as this has been shown to relieve thirst better than the administration of fluids through a tube.