Gum disease is a chronic bacterial infection of the gums and the bone surrounding the teeth. This disease can occur at any age and can affect one tooth or several teeth at the same time.
The main cause of gum disease is dental plaque, a sticky mass of bacteria, that constantly accumulates on the teeth surfaces. These bacteria can create toxins that lead to gum inflammation and subsequent damage to the bone surrounding the teeth.
In the early stage of gum disease, called gingivitis, the gums become red, swollen and bleed easily. Gingivitis can be reversed since the bone and connective tissue that hold the teeth in place are not yet affected. If gingivitis is left untreated, the bacteria may spread to the gum tissues and bone supporting the teeth. This is known as periodontitis, or periodontal disease.

Good oral hygiene reduces the risk of gum disease across all ages. The following factors increase the risk of developing gum disease:
- Poor toothbrushing and poor interdental cleaning, either irregular or improper techniques
- Smoking, as it affects your body’s ability to repair damaged gum tissue
- Uncontrolled diabetes, which affects blood sugar levels and the body’s response to infections
- Long-term medication such as calcium channel blockers for hypertension, immunosuppressant medication, oral contraceptives, steroids, anticonvulsants and chemotherapy
- Crooked teeth with poor access for oral hygiene
- Hormonal changes such as during pregnancy
- Genetic factors predisposing to gum disease
- Compromised immunity due to human immunodeficiency virus infection or cancer treatment
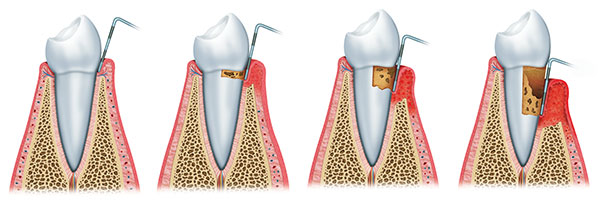
Gum disease often goes unnoticed at the early stage; consequently, it is important to be aware of the following signs and symptoms:
- Bleeding gums when brushing or flossing teeth
- Red and swollen gums
- Dull ache of the gums and teeth
- Bad breath that does not go away
- Spaces between teeth which are previously not present
- Pus formation between teeth and gums
Gum disease can be prevented. Here are some suggestions to help keep teeth, gums and the supporting bone structures healthy:
- Brush your teeth at least twice daily, for two minutes each time, and floss regularly
- Visit a dentist regularly for routine check-up and professional cleaning
- Do not smoke or use tobacco products
 Treatment modality for gum disease depends on the severity of the disease. Nonsurgical therapies that control bacterial plaque are utilised for mild and moderately severe forms of the disease. Surgery may be indicated in the advanced stages of disease to improve access for debridement and to restore supporting tissues
Treatment modality for gum disease depends on the severity of the disease. Nonsurgical therapies that control bacterial plaque are utilised for mild and moderately severe forms of the disease. Surgery may be indicated in the advanced stages of disease to improve access for debridement and to restore supporting tissues
Nonsurgical therapies include:
-
Scaling and polishing
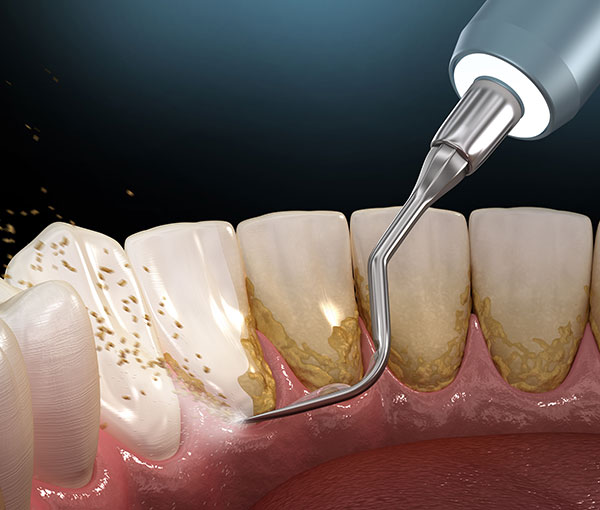
Dental plaque that is built-up on teeth over time will harden to form calculus, commonly known as tartar. Calculus can only be removed by professional cleaning by a dentist or dental hygienist. A dentist uses an ultrasonic scaling device to remove plaque, calculus and food debris from above and below the gum line, and hand instruments to remove residual deposits on the teeth and root surfaces to make them smooth to prevent plaque accumulation.
-
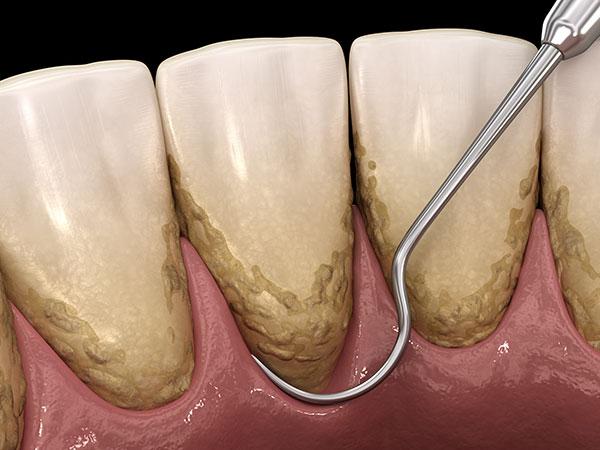
Root planing
It requires special periodontal hand instruments to remove tough calculus and bacterial deposits along the root surfaces, usually under local anaesthesia. Root planing may be required when calculus is deeply lodged and loss of attachment on teeth has occurred.
- If deep periodontal pockets associated with active periodontitis persist after initiating nonsurgical periodontal treatment, periodontal surgery will be recommended. Surgery allows the deep pockets of infection or plaque and calculus to be accessed for thorough debridement. The procedure involves raising a gum flap on the affected teeth to remove calculus and stimulate periodontal tissue healing. Bone or tissue graft material may be used in conjunction with collagen membranes in a technique known as guided tissue regeneration.