Wisdom tooth removal
Wisdom teeth also known as the third molars are situated at the back of the mouth. These teeth are normally the last teeth to erupt and appear from the late teens to early twenties, a period usually identified with the onset of maturity and the acquisition of wisdom. Most people usually have four wisdom teeth, two in the upper jaw and two in the lower jaw. Some may be congenitally missing.
These teeth are bonuses to the mouth if they are healthy and properly positioned. In most cases though, wisdom teeth are misaligned or impacted and thus require surgical removal. Poor alignment of wisdom teeth may affect or damage adjacent teeth, the jawbone or nerves in the jaw.
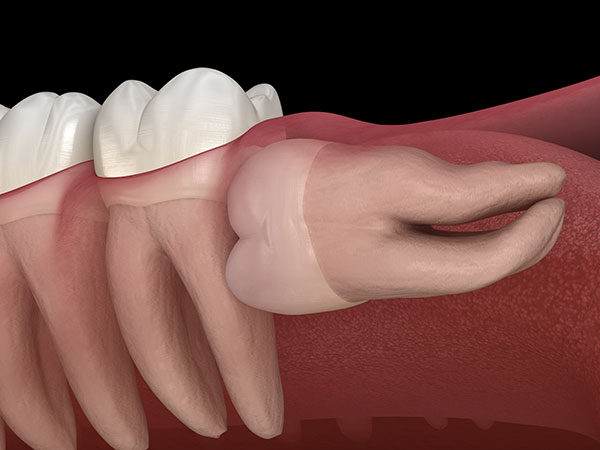
Wisdom teeth impaction occur when they are partially or entirely trapped under the gum and/or the jawbone. Partial eruption of the wisdom teeth may trap food and cause bacterial accumulation. This can lead to tooth decay and gum infection, known as pericoronitis, affecting both wisdom teeth and the neighbouring teeth. An impacted wisdom tooth may also grow into fluid-filled sacs, developing cysts and damaging the surrounding
jawbone, teeth and nerves.
These associated conditions may require complex treatment if left unattended. They can develop silently without symptoms in the early stages. Therefore, it is advisable to schedule a dental visit pre-emptively to identify any wisdom teeth conditions and allow for timely treatment.
During your visit, the dentist will examine your mouth and take a dental panoramic radiograph to evaluate the position of your wisdom teeth and determine if removal is required.
A fully erupted wisdom tooth can be removed via simple extraction. However, an impacted wisdom tooth requires surgical removal. Removal of a wisdom tooth can be performed under anaesthesia to numb the surrounding tissue. The type of anaesthesia, local or general, depends on your health condition, the number of wisdom teeth to be removed and the level of surgical complexity. After anaesthesia is administered, the buried wisdom tooth is surgically exposed and extracted as a whole, or sectioned and removed in multiple fragments.
After surgery, some minor bleeding from the wound is expected. Residual oozing may occur for a few hours. Mild swelling and bruising in the face and neck are common, this may increase over the first 72 hours. This should subside thereafter.
Ice packs and pain medication prescribed by the dentist or oral surgeon should help manage the pain. It is recommended to avoid excessive spitting or rinsing after surgery, to maintain satisfactory oral hygiene and to consume soft food for a few days following surgery.
Dental implant
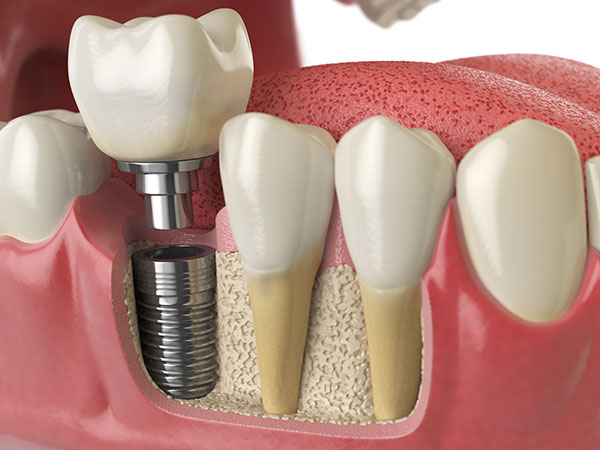
A dental implant is a titanium screw that is surgically inserted into the jawbone to replace a missing tooth. It serves as a foundation for an implant crown, which restores the space created following the loss of a natural tooth. It improves function, appearance and likely speech. It may also be used to improve the retention of dentures.
For an implant to be successfully placed, there must be adequate remaining bone in the jaw to hold the implant. The amount of bone that is available for implant is often determined by the existing bone anatomy and vital structures in the vicinity such as maxillary sinuses, in the upper jaw, and nerve bundles, in the lower jaw. When the necessary factors have been considered, an implant of a suitable size may be selected, and you can be on your way to starting your implant treatment.
At TTSH, implants are managed by a team of specialists consisting of the oral surgeon, periodontist and prosthodontist. The treatment is carried out in three stages over a minimum period of four months. This may vary depending on the case complexity and the need for additional bone grafting.
Phase 1: Treatment Planning
The specialist will examine your overall oral condition and take several dental radiographs to determine the location of the vital structures and bone volume for an individualised treatment plan.
Phase 2: Surgical Treatment
It involves making a small incision on the gums to place the titanium implant into the jawbone. If you had previously lost your tooth through chronic infection, the resultant bone loss will need to be replenished either with bone harvested from other parts of your jaw or with commercially prepared bone.
The surgical stage is performed under anaesthesia to numb the surrounding tissues. The type of anaesthesia, local or general, depends on your health condition and the level of surgical complexity.
Phase 3: Restorative Treatment
When the implant fixture is integrated with bone, the appropriate prosthesis will be fabricated for you.